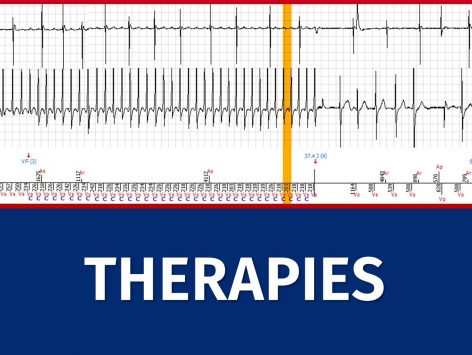
In this chapter pertaining to therapies, we no longer describe the counting of events which has been detailed in the corresponding chapter. Similarly, discrimination will not be discussed.
The tracings herein will be presented logically beginning with ventricular fibrillation, followed by tachycardias observed in the VT zone. We will describe the sequence of therapies that are called upon according to the programming of the device.