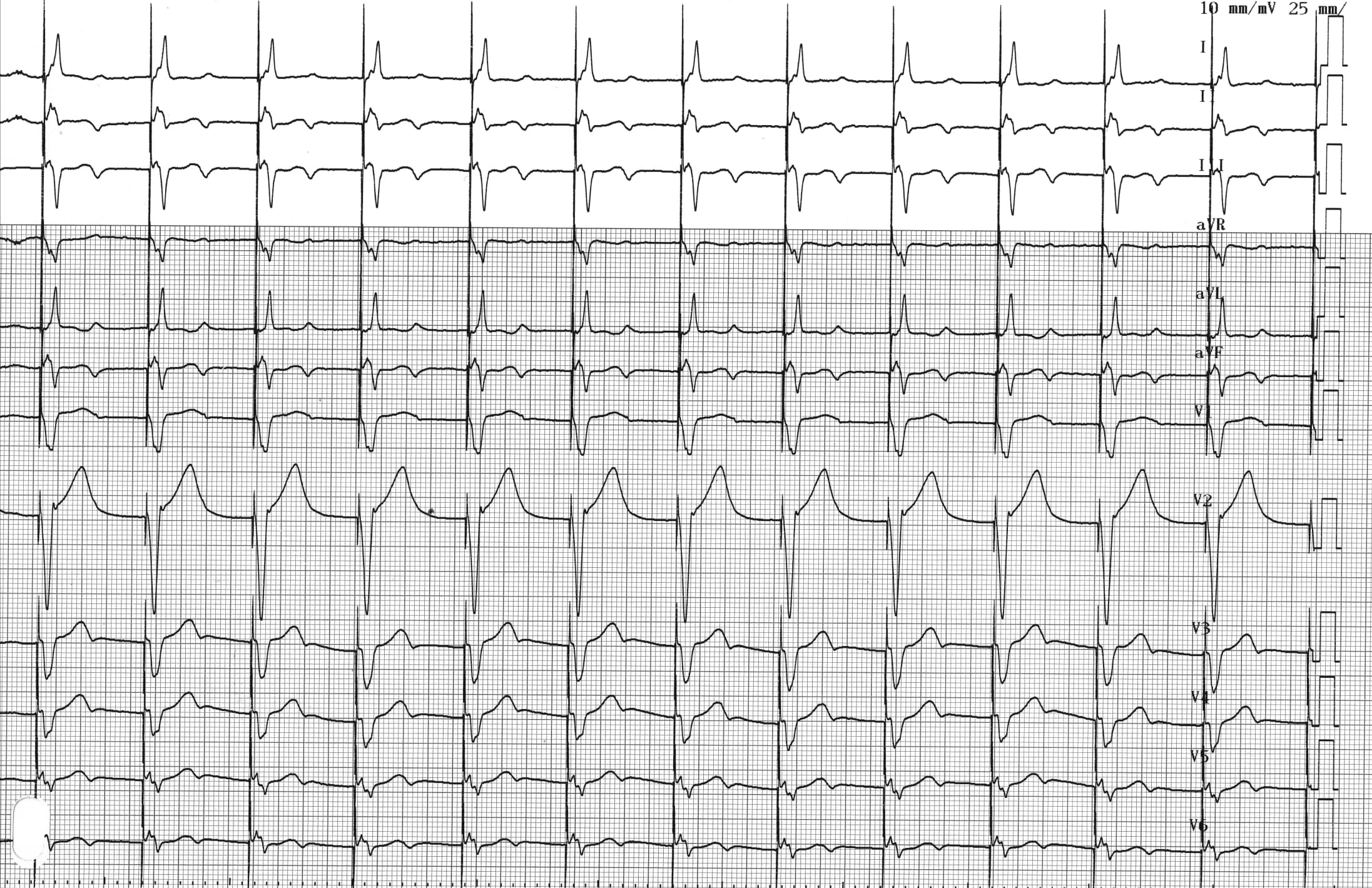
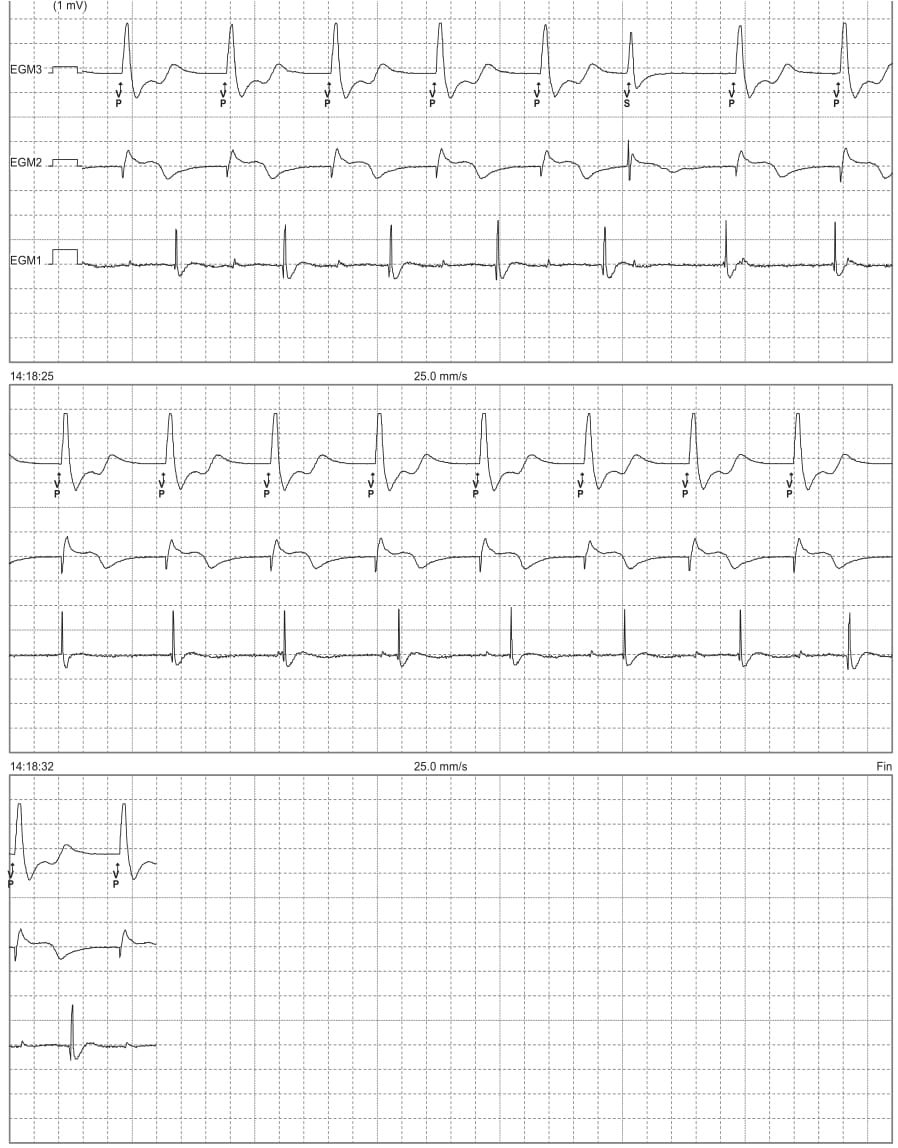
Patient: 69-year-old man implanted with a Medtronic dual-chamber pacemaker following repeated syncopes due to sinus node dysfunction; the 2 pacing leads are well positioned with normal pacing impedances, correct sensing and satisfactory pacing thresholds; 3 days after implantation, pacemaker evaluation; programming of various pacing modes and recording of tracings; for this first tracing, device programmed to VVI mode 70 bpm;
Case Summary
0 of 1 Questions completed
Questions:
Information
You have already completed the case before. Hence you can not start it again.
Case is loading…
You must sign in or sign up to start the case.
You must first complete the following:
Results
Results
0 of 1 Questions answered correctly
Time has elapsed
Categories
- Not categorized 0%
-
VVI mode
ECG 3A: On this tracing, one can distinguish ventricular pacing at 70 bpm; there is a possible 1:1 atrial activation at the end of the T wave relative to the ventricles; probable retrograde atrial activity (negative in inferior leads);
ECG 3B: In VVI mode, there are no atrial sensing markers; however, one can observe on the atrial EGM the presence of an atrial activity located remotely from each ventricular pacing corresponding to a very likely retrograde conduction;
Comments: The VVI mode provides a single chamber pacing at the programmed pacing rate (lower rate), unless inhibited by a sensed event. Sensing applies only to the ventricle. The timer resets itself after each ventricular sensed event. The VVI mode can also be programmed in a dual chamber pacemaker. For this patient, programming of the lower rate is essential. Indeed, at 70 bpm, the lower rate is too high and one observes a permanent ventricular pacing with reversal of the physiological atrioventricular activation sequence. The electrocardiogram demonstrates retrograde conduction which may aggrevate pacemaker syndrome. Atrial contraction occurs while the atrioventricular valves are closed, causing a retrograde flow to the pulmonary veins and the vena cava. Pacemaker syndrome results from a complex combination of hemodynamic, neurohumoral and vascular alterations secondary to loss of atrioventricular synchronism. A sometimes very disabling symptomatology associated with increased atrial pressure and venous pressure can include dyspnea, orthopnea, pulsations in the neck and chest, palpitations, chest pain. At 40 bpm, the lower rate would have been lower than the lowest intrinsic rate and the patient would not have been paced.
This allows
- reducing consumption and prolonging the life of the battery,
- avoiding retrograde conduction,
- pacing only upon occurrence of a paroxysmal conduction disorder.
Take-home message: Pacemaker syndrome corresponds to the presence of a repeated sequence: ventricular pacing (pacing artifact and wide QRS) and retrograde atrial conduction (negative P’ waves in the inferior leads). Atrial contraction may occur during mitral valves closure, which can lead to a variable but disabling symptomatology
- 1
- Current
- Review
- Answered
- Correct
- Incorrect
-
Question 1 of 1
1. Question
Regarding this ECG, which answer(s) is(are) true?
CorrectIncorrect